President Obama Should Look to Europe, Not the NHS
Debate on US health care needs realism, not propaganda.
The claims by both sides in the emerging furore on US health system reform and the value of government-run systems such as the NHS are clouded in ideology and misrepresentation, according to independent think tank Civitas.
- The NHS is not ‘evil’ (Sarah Palin), nor leaves the old and disabled “to die” (IBD), nor something ‘not to be wished on anyone’ (Daniel Hannan).
There are plenty of people who will have received world-class health care from the NHS and its staff and – as the Twitter campaign £welovethenhs shows – are very grateful for it. - The NHS is not ‘loved more than words can say’ (Sarah Brown), nor is it a service where ‘quality is as good as anywhere in the world; and where outcomes are as good as anywhere in the world’ (Andrew Lansley).
In an individual ward or hospital this claim may stand up, but across the board it does not. The evidence suggests European health systems outperform both the NHS and the US. (see table below)
‘The NHS is neither deity nor dinosaur’ said James Gubb, Director of the Civitas Health Unit, ‘but if the United States is serious about health reform and providing universal coverage, it should look to Europe, where systems are more competitive, responsive and patient-led than the NHS; and where coverage is based on insurance, not taxation.’
THE NEED FOR REFORM
All sides acknowledge the US health system is in big trouble:
- On most system-wide measures of health outcomes, the US fares poorly vis-a-vis other countries. On mortality amenable to health care – deaths from certain causes before age 75 that are potentially preventable with timely and effective health care – the US is the worst performing in the developed world (see table below).
- Over the last 35 years health spending in the US has risen by 9.8 per cent versus 7.2 per cent elsewhere in the US economy, which has made health care unaffordable to many. Forty-eight million people are currently uninsured.
- Employers are often burdened with a large part of the cost of health insurance, making them uncompetitive in world markets. Health care costs add over $1,500 to the manufacturer’s cost of every car made in the US, for example.
- If governments were forced to report on their financial statements the liabilities they face resulting from contractual commitments to provide health care for retired employees, nearly every city and town in the US would be bankrupt.1
Something, clearly, needs to be done. There are lessons the US can learn from the NHS:
- Universality.
In a free society, out of compassion for fellow human beings and to give people an equal chance to participate fully in society, we demand that everyone has access to a decent package of health care.
Universality has wider efficiency gains, through spreading risk – just as having mandatory car insurance does. - General practice. It is widely acknowledged that family practice medicine is in under-supply in the US, resulting in fragmented care and more serious problems cropping up further down the line, particularly for patients with chronic diseases and multiple conditions.
- Cost-effectiveness evaluations by NICE provide a good impression of value, which is essential to judging the efficacy of treatment.
‘LESSONS’ TO AVOID
But the NHS is far from the ‘perfect’ health system. The outcomes it engineers, in terms of equity, patient satisfaction and health, may be better than the US, but typically are worse than Europe:
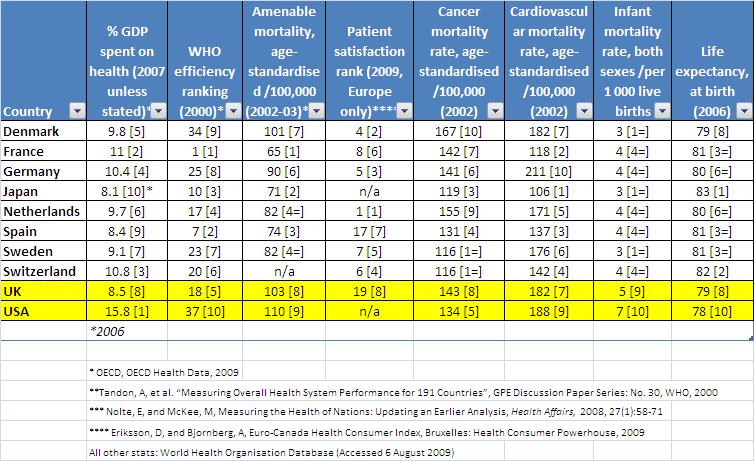
In addition:
- Inefficiency is rife. NHS productivity has fallen by 4 per cent over the past decade, according to the Office for National Statistics.
- Funding gaps are in evidence, resulting in rationing of treatment. Just today (14 August 2009) it was reported that some 1,000 cancer patients were denied drugs that may be clinically effective.
- Health inequalities have actually widened under the Labour government. The gap in life expectancy between the most and least deprived areas in England is nearly ten years (for men) and has increased in recent times.
As Peter Davies and James Gubb argued in a recent Civitas publication, Putting Patients Last, the ‘customer’ of the NHS too often is not, in fact, the patient, but the minister.
With the government having a monopoly on funding and resource allocation, and feeling the constant need to intervene to be seen as ‘accountable’ to the taxpayer, success is judged more by meeting central targets than by the end-goal of providing high quality care for the patient.
EUROPEAN IDEAS
In an ICM poll in 2006, 65 per cent of respondents agreed the NHS was the right idea when it was introduced in 1948, but that Britain has changed and we need a different system now; 80 per cent, for example, agreed it shouldn’t matter whether hospitals or surgeries are run by public, private or voluntary organisations, so long as everyone including the poorest has access. Perhaps it is the ideals of solidarity and universality that attract such support, rather than the NHS itself?
There is increasing recognition that we need health systems that are competitive, responsive and consumer-driven, with clear metrics of value (cost and health outcomes).
The challenge for the US is to embrace these values within a universal insurance framework. The NHS does not provide such a model, and it is questionable whether the solution will require a public plan to compete with private insurers, as President Obama is proposing. Such a role for government is not considered necessary in the most competitive universal, insurance-based systems in Europe, such as the Netherlands and Switzerland.
Instead, they rely on certain core principles:
- All individuals (not employers as in the US) are obliged to pay into a health insurance plan offered by a variety of insurers; who can compete on price, deductibles and service offerings. But:
- Insurers are obliged to accept all the applicants that choose them;
- The government both defines the mandatory minimum package, and pays for top ups for those on low incomes or with excessive health risks.
Crucially, this ensures the consumer – the patient – controls the purse strings, not the government or, for that matter, employers.
As Regina Herzlinger, Nancy R. McPherson professor of business administration at the Harvard Business School, has said “the Swiss system provides important lessons for the United States about consumer-driven health care.”
James Gubb, director of the health unit at Civitas said: ‘Gordon Brown’s twittering, David Cameron’s call for “pride in the NHS” and Daniel Hannan’s claims that he “wouldn’t wish the NHS on anyone” all miss the point slightly. Outcomes are better in Europe; and, with a system already based on insurance, the United States would do well to look across the channel for solutions.’
1. Christensen, C, Grossman, J, Hwang, J, The Innovator’s Prescription: A disruptive solution for health care, McGraw-Hill, 2009
For more information contact James Gubb on: 020 7799 6677 / 079 3024 3570
Notes for Editors
i. Civitas is an independent social policy think-tank. It receives no state funding either directly or indirectly and has no links to any political party.
ii. ii. You can find a link to Civitas briefings on various European health systems, including the Netherlands and Switzerland here.
iii.‘Putting Patients Last: How the NHS keeps the ten commandments of business failure’ by Peter Davies and James Gubb was published by Civitas in July 2009, at £10.25 inc. pp. ISBN: 978-1906837099. Buy from Amazon.
